|
We performed a complete echocardiographic examination identifying the patient with left ventricular ejection fraction (EF) about 64%, tricuspid valvuloplasty, and no shunt following repair of the atrial septal defect. Her bedside ECG showed sinus rhythm ( Figure 1). Cardiac rhythm is regular with no murmur. Her blood pressure at presentation was 109/75 mmHg, heart rate 96 bpm, afebrile, oxygen saturation (SaO 2 99%). She has no history of smoking or drinking. She was without hepatitis and tuberculosis. She was with no history of hypertension and diabetes mellitus. She had undergone tricuspid valve plasty for nonrheumatic tricuspid valve insufficiency and pericardial patch technique for the congenital atrial septal defect in 2018. Our case complied with the Declaration of Helsinki and was approved by our local research ethics committees of the first affiliated hospital of the university of science and technology of China, with the patient giving written informed consent. We present the following case report in accordance with the CARE reporting checklist (available at ).Ī 54-year-old female who had experienced choledochotomy and cholecystectomy for Choledocholithiasis and cholecystolithiasis went to the emergency department at 14:33 on July 16, 2020. It is crucial to avoid mismanagement/misdiagnosis in patients with wide QRS complex tachycardia and rates above 200 beats per minute. Through observations of the dynamic changes during and after amiodarone treatment, we made the diagnosis. Amiodarone was administered under the guidance of a cardiovascular physician. Meanwhile, we did RS/QRS ratio in lead V6. 
We did Brugada’s stepwise approach and the VT score for the diagnosis. AFL with 1:1 AVC must be differentiated from rapid arrhythmias, such as ectopic atrial tachycardia (AT), AV node reentrant tachycardia (AVNRT), and ventricular tachycardia (VT). 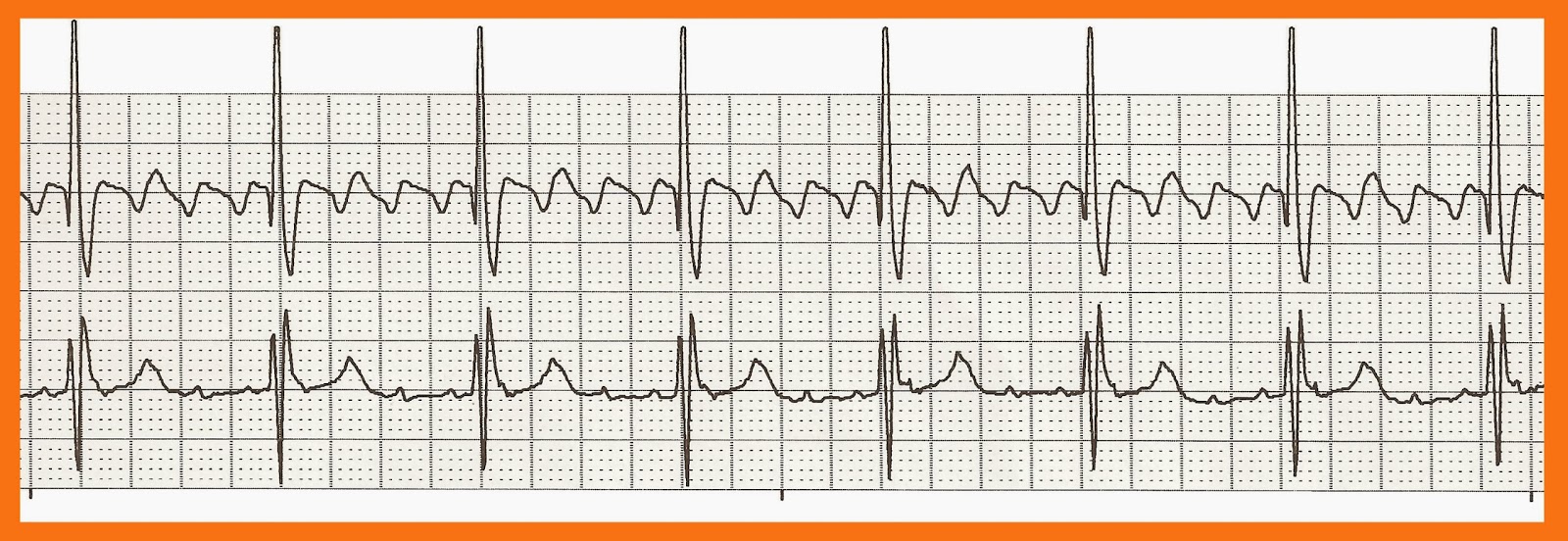
AFL with 1:1 wide QRS tachycardia may present a clinical diagnostic challenge. Her electrocardiogram (ECG) during the arrhythmia attack revealed wide QRS tachycardia with rates of 250 beats per minute. The patient underwent a traditional pericardial patch technique for the atrial septal defect 2 years ago. Received: 10 January 2021 Accepted: 02 March 2021 Published: 30 June 2021.Ī patient developed atrial flutter (AFL) with 1:1 rapid wide QRS atrioventricular conduction (AVC). Keywords: Atrial flutter (AFL) 1:1 atrioventricular conduction (1:1 AVC) electrocardiogram (ECG) One should be conscious of the different presentations of AFL with 1:1 wide QRS AVC to avoid misdiagnosis and mismanagement. Through observation of the changes of ECG before and after amiodarone, we can make the diagnosis. In our study, we also verify that the RS/QRS ratio in lead V6 is beneficial to differentiate supraventricular tachycardia (SVT) with a right bundle branch block (RBBB) pattern from VT. Brugada’s stepwise approach and the VT score can assist clinical physicians in making the diagnosis. AFL with 1:1 AVC is an uncommon but challenging arrhythmia. Retrospectively, the rapid arrhythmia ECG was diagnosed as AFL with 1:1 rapid wide QRS AVC. The AFL rate was the same as the rate of rapid arrhythmia attack. 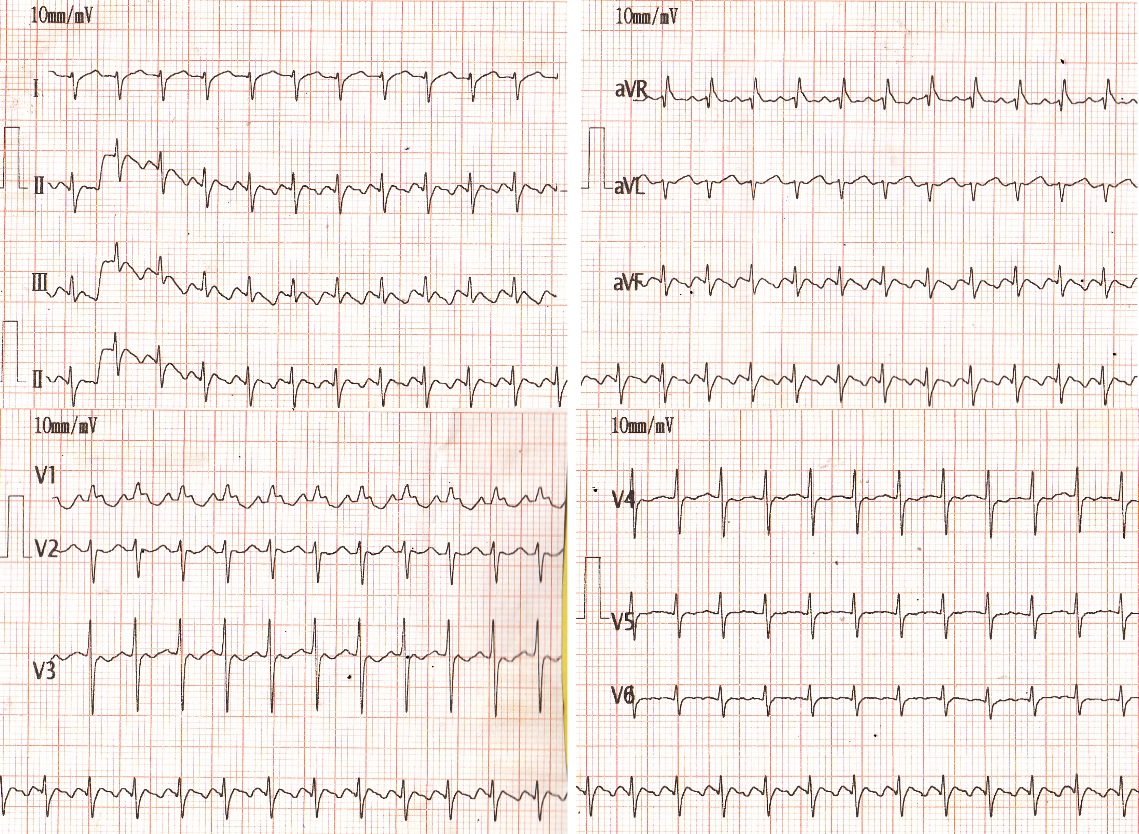
Through observations of the dynamic changes during and after amiodarone treatment, the electrocardiogram (ECG) showed AFL with 2:1 AVC. Finally, amiodarone was administered under the guidance of a cardiovascular physician. The result also suggested that the wide QRS AV tachycardia was not VT. Meanwhile, we did RS/QRS ratio in lead V6, and the result showed the rate of 0.369 (<0.41, cut off 0.41). Secondly, we made Brugada’s stepwise approach to exclude VT. 
Firstly, we calculated the VT score, and the result showed score 1. We did Brugada’s stepwise approach and the ventricular tachycardia (VT) score for the diagnosis. We present the diagnostic and analytical strategy for a patient who developed a paroxysm of AFL with 1:1 AVC.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
